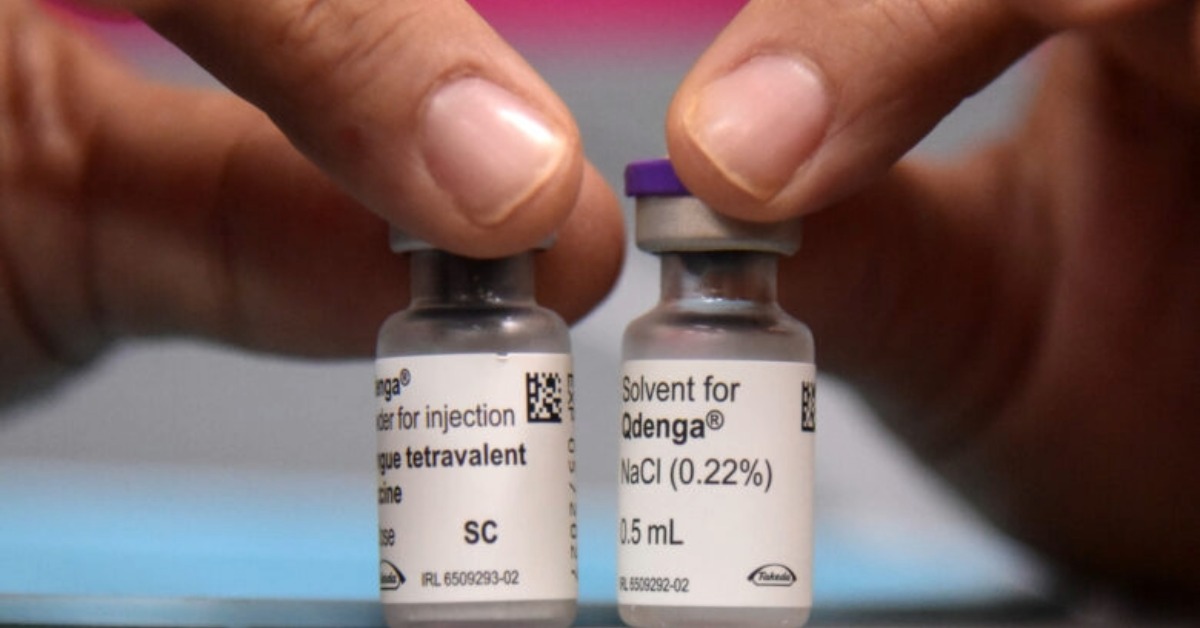
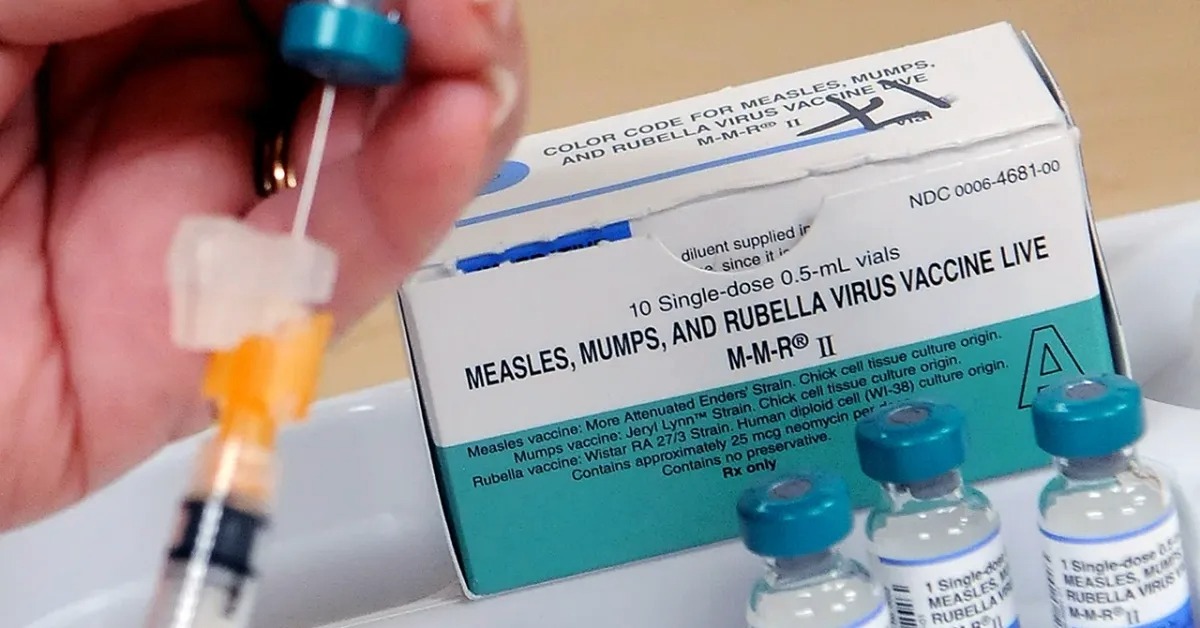
A warning from the Pan American Health Organization is putting a routine hospital task under a harsher light. Nearly 70% of medical waste in Latin America and the Caribbean is estimated to be handled poorly, even though some of it can spread infection or release toxic pollutants. Mexico already has rules on the books, but the regional alert raises a harder question: how well are those rules enforced inside hospitals, clinics, labs, and the waste chain that follows them?
A regional warning with local weight
Mexico is not named as a worst-case scenario in the regional warning. Still, the message lands close to home. The Pan American Health Organization says nearly 70% of hospital waste in Latin America and the Caribbean is not managed properly. At the same time, 13 countries in the region are updating their strategies and technical capacity to ensure safer handling and disposal. For Mexico, the issue is larger than sanitation. It touches on infection control, worker safety, and nearby communities. It also affects trust in a health system that must protect people after care is delivered.
This is also a story about volume. Hospitals, clinics, labs, and related services generate waste every day. Most of it is ordinary trash. But the World Health Organization says about 15% is hazardous. In lower-resource settings, that risky share is often not separated from the rest. That means the problem can become larger in practice. When facilities fail to sort material at the point of generation, risk moves outward. It can reach cleaners, transport workers, landfill staff, patients, and the environment itself.
Why hospital waste is different
The dangerous part of the stream includes sharps, blood-contaminated materials, lab cultures, pathological waste, and some chemicals or pharmaceuticals. PAHO says much of the poorly managed waste in the region ends up in landfills or is discarded without control. Open burning and low-temperature incineration can add another problem. They may release dioxins, furans, and fine particles into the air. WHO also warns that harmful microorganisms, including drug-resistant ones, can escape from health facilities into the environment. That is why waste management is not a side issue. It is part of basic public health and environmental protection.
The problem is easy to underestimate because it often begins with ordinary routines. A syringe is used. A dressing is changed. A lab sample is processed. A container is moved down a hallway. If the sorting is wrong at the start, the error can travel through the rest of the chain. By the time waste reaches storage, transport, or disposal, fixing that error is harder and more expensive. In that sense, medical waste is not only a disposal issue. It is a management issue that starts inside the treatment room.
What Mexico already has on paper
Mexico is not starting from zero. The country has a federal standard, NOM-087-SEMARNAT-SSA1-2002, which has been in force since 2003. It governs the classification and handling of residuos peligrosos biológico-infecciosos (RPBI). In plain terms, the rule covers the full chain. That includes separation, packaging, storage, collection, transport, treatment, and final disposal. The regional warning, then, is not only about writing rules. It is about whether every part of that chain works every day.
That question matters because weak waste handling often hides in routine operations. A facility may have a rulebook and still struggle with training, supplies, space, contractors, or oversight. A smaller center can face its own limits. A busy hospital can face volume. When hazardous and ordinary waste are mixed, the practical burden grows. More material may need special handling, and mistakes become harder to reverse once the waste leaves the place where it was generated.
The wider health gap
The regional warning also fits a broader global picture. WHO and UNICEF estimate that only 61% of hospitals worldwide had basic health-care waste services in 2021. A separate WHO analysis found that one in three health facilities did not safely manage health-care waste. Those numbers help explain why this is still treated as a system issue rather than a one-off failure. The gap is not only about disposal. It is about the basic infrastructure that keeps medical care from creating new risks.
For expats and other international readers, this can sound like a technical issue. It is not. Hospital quality is usually judged by doctors, beds, and wait times. Waste management is less visible, but it sits in the same safety chain. It affects exposure risk inside facilities and environmental conditions outside them. Safe care does not end when treatment ends. It continues through segregation, sealed storage, reliable transport, proper treatment, and final disposal away from open dumping or poor burning practices.
The latest warning does not prove that Mexico matches the regional average. But it does raise a fair question about how consistently Mexican facilities meet the standard already on the books. That is a question worth watching, because the consequences reach far beyond the hospital door.
With information from Pan American Health Organization