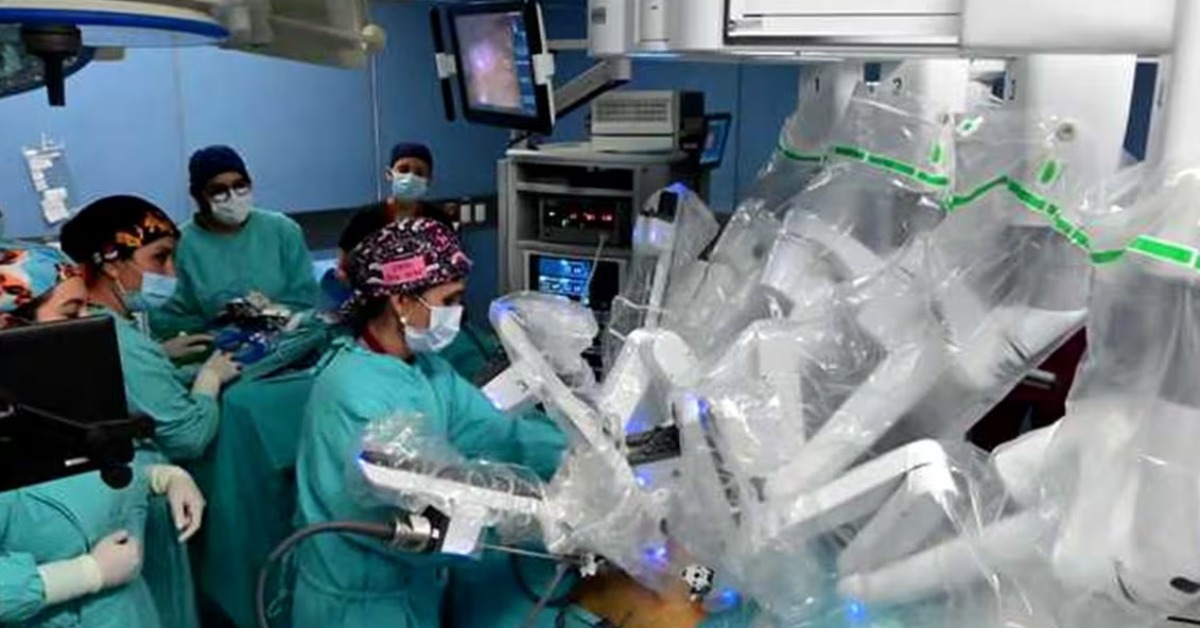
A quiet shift is underway in one of Mexico’s busiest cancer operating rooms. At INCan, surgeons are using a robotic platform for complex procedures that once meant large incisions and long recoveries. Doctors say many patients now walk and eat within a day, and some go home in two. But the robot is not for everyone, and outcomes still depend on tumor type, stage, and team experience. Here’s what the program is doing, who is being selected, and what evidence the institute says it is still building.
Inside INCan’s robotic surgery rollout
At the Instituto Nacional de Cancerología (INCan) in Mexico City, robot-assisted surgery is becoming routine. The institute says the program began in August 2024. Clinicians report it is now nearing 300 procedures. Several services use the platform, including colon and rectum, urology, gynecologic oncology, and thoracic surgery. Teams describe cases in the rectum, prostate, and endometrium. They also report procedures in the lung, liver, pancreas, and upper digestive tract. Surgeons still aim for the basics: remove the tumor and leave clear margins. The difference is the access. Many cases use ports about 8 millimeters in diameter rather than a long incision. That can reduce wound healing demands. Clinicians report that many patients walk and begin oral intake within 24 hours. Some leave the hospital within 24 to 48 hours. The strongest case, they argue, is deep pelvic surgery. In that space, nerves and sphincters sit close to the tumor, and visibility matters.
The “robot” does not operate on its own. The surgeon controls every move from a console. The system provides a magnified 3D view and instruments with wrist-like joints. Motion scaling can turn a large hand movement into a small tip movement. Tremor filtering can steady fine dissection. Those features can help in narrow spaces and around delicate vessels. Setup matters, too. The patient is positioned, and ports are placed in planned locations. Robotic arms then dock to the ports, and the camera and tools are introduced. A second surgeon stays at the bedside to assist and to manage urgent steps. The team also includes anesthesia, scrub staff, technical support, and biomedical engineering. Early in the rollout, the institute reported starting with a small group of certified surgeons. It has aimed to expand that pool over time. INCan says it tracks workflow details, such as docking time, because consistency affects safety.
What changes for recovery and function
The institute highlights benefits it can measure. Surgeons describe low blood loss in many cases. That can reduce the need for transfusions and related risks. They also report earlier walking and earlier oral intake after major procedures. Shorter stays matter for patients and hospitals. INCan clinicians can describe two to three days in many robotic cases. Open surgery often requires longer admissions, especially after complex pelvic work. Clinicians note that many patients arrive with locally advanced disease, which can make pelvic dissection more demanding. Fewer hospital days can also reduce exposure to hospital-acquired infections. In rectal cancer, clinicians say finer control can help protect the anal sphincter. For some patients, that can mean avoiding a permanent ostomy. In prostate surgery, they emphasize nerve-sparing dissection. That can affect urinary control and sexual function. Quality-of-life outcomes often depend on details that are hard to see in a chart. These outcomes do not end at discharge. INCan says it follows patients for complications, recovery, and cancer control. The goal is to compare results over time and to identify where the robot adds value.
Who qualifies and why evidence matters
Robotic surgery is not offered to every patient. INCan clinicians describe a strict selection. They often avoid very bulky tumors and extensive metastatic disease. Decisions are made through multidisciplinary review, not by a single surgeon. Surgery is treated as one step in a longer plan. Some patients will still need chemotherapy or radiation. Clinicians also stress that complications remain possible. Leaks, bleeding, and infections can occur in any major operation. Conversion to an open approach is still part of safe practice when anatomy or bleeding demands it. International research also shows that a blanket “minimally invasive” promise can be misleading. In early-stage cervical cancer, minimally invasive radical hysterectomy has been linked to worse survival than open surgery. Guidelines in several settings shifted toward open surgery for that reason. Volume and team training can also shape outcomes. INCan says its goal is to avoid assumptions. It is documenting recurrence and survival alongside recovery metrics.
What this means for patients in Mexico
For many expats living in Mexico, the key issue is access. INCan is a public referral center in Mexico City. Early program announcements framed robotic surgery as a way to expand access to advanced care for patients without health insurance. Expats may reach robotic surgery through different systems. Some use IMSS or ISSSTE. Others rely on private insurance or pay out of pocket. Mexico already has other public hospitals running large robotic oncology programs, and capacity differs by region. Wherever a robot is offered, the decision should stay specific to your case. Ask how often the team performs your exact operation. Ask what outcomes they track after discharge, including urinary, bowel, and sexual function when relevant. Also, ask what happens if the plan changes during surgery. A platform can improve reach and visibility, but it does not replace judgment. For patients, the practical goal is consistent: safe tumor removal, low complication rates, and a clear path back to treatment or daily life.